You twist and wind along dusty, unfinished roads in a beat up old jeep, moving through bumpy pastures. You pass horses, cattle, sheep, goats and camels and nomadic Gur communities scattered across the grasslands – for seven hours.
This is a taste of what BC Emergency Health Services (BCEHS) Director of Clinical Practice, Joe Acker, experienced earlier this month when he travelled to Mongolia to support the country’s emergency medical services (EMS). It was a rare opportunity for Acker to immerse himself in another culture, observe, participate and offer insight from his 30 years of experience as a paramedic, clinical practitioner and leader with BCEHS.
As one of the largest ambulance services in North America with more than 45 years delivering paramedic care, BCEHS has developed effective ways to manage patient care across a vast geographical area. Not only is its service area nearly one-million square kilometres in size, the terrain variations are significant. These BC conditions are similar to Mongolia, so Acker felt well-positioned to share BCEHS best practices and innovative approaches to patient care with Mongolia EMS.
During his 12-day visit, Acker kept a tight schedule that included delivering medical training to the Mongolian National Emergency Management Agency, working with ambulance doctors and sharing pre-hospital care and meeting with health system decision-makers to propose new models for emergency medical services in Mongolia.
Here are some of Acker’s key observations:
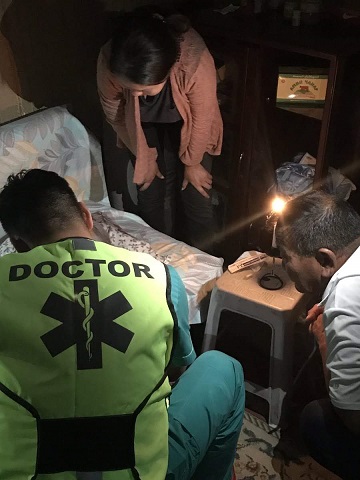
- In Mongolia, ambulances are staffed by a driver and a doctor. The drivers have no medical training and the doctors are generally new graduates with no specific pre-hospital or emergency medicine training. We proposed the creation of a short curriculum to teach drivers to support doctors with basic patient care, and a short course for doctors in prehospital trauma care and resuscitation.
- A strength of the Mongolian system is the ability of ambulance doctors to perform procedures on patients at home without transporting them to hospital. We observed a doctor stitching up a patient on the side of the road. We also attended several calls where the doctor was able to write a prescription or make a referral without the need to transport the patient to the emergency department.
- A highlight of the trip was a school in Bayangol where the students welcomed us with traditional music, dancing and singing, and hosted us for lunch so the students could practice their English-speaking skills. It was incredibly heartwarming.
- We passed through numerous nomadic Gur communities during our travels and gained an appreciation for the remoteness of Mongolia and challenges they have in health care. We take so much of what we have here for granted.

This
Roadside to Nationwide project was funded by the World Health Organization, Australia’s Griffith University and the government of Mongolia. Acker was joined by Vancouver Fire Chief Darrell Reid and Australian researchers. The team presented their observations and recommendations at the Society of Emergency Medicine Symposium held at the Mongolian National Parliament.
