Stimulate: If you suspect someone might be having an opioid overdose, start by stimulating them to confirm that they are unresponsive. Shout at them – use their name if you know it. Next do a trapezius squeeze (squeeze the nailbed of the finger) or pinch the webbing between their thumb and fingers to see if they respond to pain. Always tell someone what you are going to do before you touch them.
If the person does not respond to sound or pain, then it is a medical emergency.
Call 9-1-1. If you are alone, you can put the phone on speaker. Remember, you will not get in trouble if you call 9-1-1 for a suspected overdose.
The call-taker will ask for:
- Your location – address, cross streets, name of business, and town or city
- Your phone number, in case you get disconnected
- What the problem is
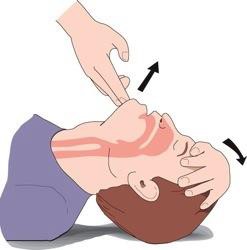 Airway
Airway: Check the person’s mouth for any obstructions. Items like gum, dentures, or a syringe cap could be preventing them from breathing properly. Remove any obstructions. Once you’ve confirmed the mouth is clear, tilt their head back – this opens their airway.
Ventilate: The next step is to breathe for the person.
Breaths are crucial to the overdose response. They keep the brain alive. Ventilation is the best way to reduce the risk of irreversible brain injury.
BCEHS call-takers provide step-by-step instructions on how to give rescue breaths followed by naloxone administration in a respiratory arrest or opioid overdose.
A mask is available in the
Take Home Naloxone kit to provide a barrier. You can use a piece of clothing if you do not have a mask.
Keep the person’s head tilted back, pinch their nose, and give them two breaths. You should be able to see their chest rise with each breath. Continue to give one breath every five seconds until the person is breathing on their own or first responders arrive.
If you are responding by yourself and do not have naloxone, or do not feel confident about administering naloxone, breaths are more important.
Some people may not be comfortable giving rescue breaths. In that case, call-takers can also coach 9-1-1 callers through providing chest compressions.
Evaluate: Has the person responded to your breaths?
If they are still unresponsive, continue the rescue breathing (one breath every five seconds). Now is the time to give naloxone, if you have it. If there is someone with you, have them prepare the naloxone kit.
If you do not have naloxone, or if you are alone and can’t prepare the kit, keep providing breaths until first responders arrive.
- SAVE ME instructions in the lid
- Alcohol swabs
- Gloves and a breathing mask to protect the responder
- Three Vanishpoint® syringes
- Pill bottle containing three ampoules of naloxone
- An overdose response information form to be completed after the naloxone has been used.
Naloxone comes in glass ampoules that need to be opened.
- Hold the ampoule by the top and swirl to bring all the medication to the bottom. Gently but firmly snap the ampoule top off, away from your body. The plastic amp snapper is there to protect your fingers.
- Pull the plunger to draw up the liquid.
- Inject the naloxone into a muscle. Press the plunger all the way down to trigger the safety retraction.
Evaluate: Monitor the person to see if they respond to the naloxone. Do they start breathing again? Do they regain consciousness?
If not, keep giving one breath every five seconds.
If they have not regained consciousness after three to five minutes (approximately 40 breaths), you can give a second dose of naloxone.
Monitor the person after each dose is given for three to five minutes (approximately 40 breaths) before giving additional doses.
Naloxone is a safe medication, but people who are dependent on opioids may experience unpleasant withdrawal symptoms like pain, sweating, agitation and irritability. For this reason, it is important to give the lowest dose of naloxone required to reverse the overdose. Naloxone can take three to five minutes to work, so waiting five minutes between doses is important.